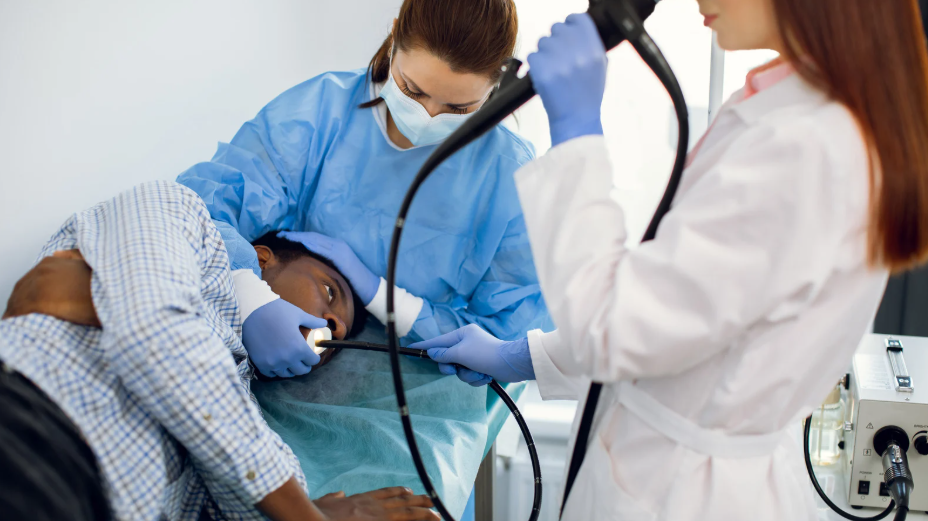
Upper endoscopy is a vital diagnostic tool used to evaluate the health of the upper digestive tract, including the esophagus, stomach, and duodenum. Patients experiencing persistent gastrointestinal symptoms such as abdominal pain, nausea, vomiting, or difficulty swallowing often benefit from professional assessment through an upper endoscopy in Baltimore. This minimally invasive procedure allows physicians to visualize internal structures directly, identify abnormalities, and obtain tissue samples when necessary. Understanding the role and benefits of upper endoscopy helps patients make informed decisions and ensures early detection of conditions that may require medical or surgical intervention.
Common Conditions Diagnosed
Upper endoscopy is used to diagnose a wide range of gastrointestinal disorders. Conditions such as acid reflux, gastritis, ulcers, Barrett’s esophagus, and tumors can be accurately identified through this procedure. Patients with chronic or severe symptoms may require the procedure to confirm diagnoses and guide treatment planning. The surgical team carefully reviews medical history, prior imaging, and presenting symptoms to determine the appropriateness of endoscopy. There are quite a few resources that can provide guidance on post-procedure activity and dietary recommendations for optimal foods. Early and precise diagnosis is essential for developing effective treatment strategies and preventing complications.
Procedure Overview
During an upper endoscopy, a flexible tube equipped with a camera and light is inserted through the mouth to examine the upper digestive tract. The procedure is typically performed under sedation to ensure patient comfort and safety. The surgical team monitors patients closely throughout the process, providing real-time evaluation of the digestive tract and performing interventions such as biopsies when necessary. The minimally invasive nature of the procedure allows for a relatively quick recovery, and patients can often return to normal activities within a day or two. By providing direct visualization, upper endoscopy offers more accurate diagnostic information than imaging tests alone.
Benefits of Professional Oversight
Professional oversight is crucial to the success and safety of upper endoscopy. Experienced physicians and surgical teams ensure that the procedure is conducted accurately and that any findings are interpreted correctly. Patients receive clear instructions on preparation, such as fasting requirements, and guidance on post-procedure care. Monitoring during and after the procedure helps identify potential complications early, including bleeding or adverse reactions to sedation. Comprehensive professional care maximizes the diagnostic value of the procedure while minimizing risks, giving patients confidence in both the process and the results.
Post-Procedure Care and Follow-Up
Recovery after upper endoscopy is generally straightforward, but professional guidance is essential to ensure safety and comfort. Patients may experience mild throat discomfort, bloating, or cramping, which typically resolves within a day. Follow-up care includes reviewing findings, discussing any necessary treatment plans, and providing guidance on diet, medications, and lifestyle modifications. Structured post-procedure recommendations help patients recover safely and support long-term gastrointestinal health. By adhering to professional guidance, patients can address underlying conditions promptly and prevent the progression of digestive disorders.
Conclusion
Upper endoscopy is a critical tool for diagnosing and managing a variety of gastrointestinal disorders. Undergoing an upper endoscopy in Baltimore with professional oversight ensures accurate evaluation, safe procedure execution, and comprehensive post-procedure care. Patients benefit from early detection of conditions, precise diagnosis, and guidance for effective treatment strategies. By combining expert evaluation with structured follow-up and patient education, the procedure supports optimal digestive health and long-term well-being, providing both reassurance and effective clinical outcomes.
